 Have you ever wondered what an X-ray is, why it’s necessary, and what it shows? Or maybe wonder why not an MRI or CT scan, and which one is better, or contrast or no contrast? In this article we will talk about different types of imaging for orthopaedic spine conditions. Most of the information was generated by our own very skilled and knowledgeable radiology technologist RT(R) Amy Hudson.
Have you ever wondered what an X-ray is, why it’s necessary, and what it shows? Or maybe wonder why not an MRI or CT scan, and which one is better, or contrast or no contrast? In this article we will talk about different types of imaging for orthopaedic spine conditions. Most of the information was generated by our own very skilled and knowledgeable radiology technologist RT(R) Amy Hudson.
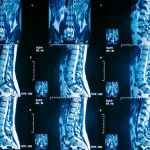
X-rays create 2D images of the body’s organs and bones. In general, X-rays show dense objects, and the denser the object the more apparent it shows up on the film. For instance, metal pops up bright white, while bones are less white. X-ray images are great for determining pathology with bones including; fractures, dislocations, arthritic conditions, and sometimes cancer. In spine the first image we utilize is often the X-ray due to its convenience and information it provides. Using these films we can visualize arthritic and degenerative changes, fractures, dislocations, alignment issues, and many other findings. It is a simple exam that provides a lot of information about the patient and can confirm the diagnosis or guide future treatment.
Another imaging study that we use in spine is the MRI (magnetic resonance imaging). MRI uses magnetism and radio waves to produce images of body structures. In spine we can utilize the MRI to visualize soft tissue anatomy that can cause pain such as a herniated disc or pinched nerve. Certain structures include; the spinal cord, spinal nerves, intervertebral discs, muscles, cartilage, inflammatory bone changes, fractures, and many other findings. An MRI can give you a massive amount of information but the key is to answer the questions of why you are ordering the MRI in the first place. For example, let’s say a patient presents to the clinic and is complaining about right leg sciatic type pain going down the back of the leg and into the foot. The physical exam points to a specific nerve being compressed in the low back on the right side. The MRI is ordered and shows a herniated disc in the low back that is compressing a nerve on the right side, and surgery is scheduled to repair the herniated disc. Thus we utilized the MRI to confirm the suspected diagnosis and also to develop a treatment plan. Another component of an MRI is whether or not to utilize contrast. Sometimes contrast can give further information when it is necessary. For instance, if a patient has already had surgery, contrast can be used to determine more accurately post-surgical changes and scar tissue. Also an important note, there are some contraindications to having an MRI performed such as cardiac pacemakers, certain metal implants, recent surgeries, and a few other contraindications. MRI is a key tool that we use often in orthopaedic spine.
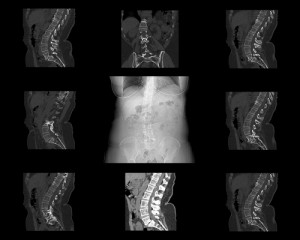 A CT (computerized tomography) scan uses a series of X-ray images taken at a variety of angles and uses computer technology to produce 3D cross-sectional images (slices) of bone, organ systems, and blood vessels. In spine CT scans show more detail than an X-ray and can help diagnose suspected spine conditions. Many spine physicians will sometimes utilize contrast with the CT to create what’s called a CT Myelogram. This requires epidural injection of dye (spinal tap). Once the dye is inserted into the spine, images are taken of the spine to reveal any injuries, spinal cord compression, spinal nerve compression or lesions, or tumors in the spine. A CT myelogram does give additional information but due to its invasiveness it is typically used only when other options are not available.
A CT (computerized tomography) scan uses a series of X-ray images taken at a variety of angles and uses computer technology to produce 3D cross-sectional images (slices) of bone, organ systems, and blood vessels. In spine CT scans show more detail than an X-ray and can help diagnose suspected spine conditions. Many spine physicians will sometimes utilize contrast with the CT to create what’s called a CT Myelogram. This requires epidural injection of dye (spinal tap). Once the dye is inserted into the spine, images are taken of the spine to reveal any injuries, spinal cord compression, spinal nerve compression or lesions, or tumors in the spine. A CT myelogram does give additional information but due to its invasiveness it is typically used only when other options are not available.
If you have neck or back pain, come see us at Prairie Spine & Pain Institute where we utilize the latest techniques to diagnose and treat spine conditions.
 About The Author: Derek N. Morrow, PA-C is a physician assistant with Prairie Spine and Pain Institute. Derek works in the clinic setting as a health care provider seeing patients. He is also utilized in the operating room as a first assist in surgery. In the clinic setting, his key function is to diagnose new patients and conduct their initial treatment. He works directly with patients to establish customized treatment programs and to monitor their progress. He also conducts history and physical evaluations for many patients. He performs many office procedures including trigger point injections, large joint injections, and bursa injections, all with the help of ultrasound guidance. He is radiologically trained, and uses his knowledge of X-ray, Ultrasound, MRI, CT, and EMG-Nerve Conduction Studies to establish a diagnosis and determine the appropriate treatment. Derek is surgically trained and plays a vital role in the procedures we perform at Prairie Spine and Pain Institute.
About The Author: Derek N. Morrow, PA-C is a physician assistant with Prairie Spine and Pain Institute. Derek works in the clinic setting as a health care provider seeing patients. He is also utilized in the operating room as a first assist in surgery. In the clinic setting, his key function is to diagnose new patients and conduct their initial treatment. He works directly with patients to establish customized treatment programs and to monitor their progress. He also conducts history and physical evaluations for many patients. He performs many office procedures including trigger point injections, large joint injections, and bursa injections, all with the help of ultrasound guidance. He is radiologically trained, and uses his knowledge of X-ray, Ultrasound, MRI, CT, and EMG-Nerve Conduction Studies to establish a diagnosis and determine the appropriate treatment. Derek is surgically trained and plays a vital role in the procedures we perform at Prairie Spine and Pain Institute.







